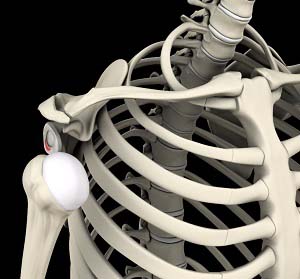
What is Shoulder Instability?
Shoulder instability is a chronic condition that causes frequent dislocation of the shoulder joint.
Causes of Shoulder Instability
A dislocation occurs when the end of the humerus (ball portion) partially or completely dislocates from the glenoid (socket portion) of the shoulder. A partial dislocation is referred to as a subluxation whereas a complete separation is referred to as a dislocation.
Risk Factors of Shoulder Instability
The risk factors that increase the chances of developing shoulder instability include:
- Injury or trauma to the shoulder
- Falling on an outstretched hand
- Repetitive overhead sports such as baseball, swimming, volleyball or weightlifting
- Loose shoulder ligaments or an enlarged capsule
Symptoms of Shoulder Instability
The common symptoms of shoulder instability include pain with certain movements of the shoulder, popping or grinding sound that may be heard or felt, swelling and bruising of the shoulder seen immediately following subluxation or dislocation.
Visible deformity and loss of function of the shoulder occur after subluxation or sensation changes such as numbness. Partial paralysis can occur below the dislocation because of pressure on nerves and blood vessels.
Treatment Options for Shoulder Instability
Conservative Treatments for Shoulder Instability
The goal of conservative treatment for shoulder instability is to restore stability, strength and a full range of motion. Conservative treatment measures may include the following:
Closed reduction: Following a dislocation, your surgeon can often manipulate the shoulder joint, usually under anesthesia, realigning it into proper position. Surgery may be necessary to restore normal function depending on your condition.
Medications: Over-the-counter pain medications and NSAIDs can help reduce the pain and swelling. Steroidal injections may also be administered to decrease swelling.
Rest: Rest the injured shoulder and avoid activities that require overhead motion. A sling may be worn for 2 weeks to facilitate healing.
Ice: Ice packs should be applied to the affected area for 20 minutes every hour.
Surgery for Shoulder Instability
When conservative treatment options fail to relieve shoulder instability, your surgeon may recommend shoulder stabilization surgery. Shoulder stabilization surgery is performed to improve the stability and function of the shoulder joint and prevent recurrent dislocations. It can be performed arthroscopically, depending on your condition, with much smaller incisions.
Arthroscopy is a surgical procedure in which an arthroscope, a small flexible tube with a light and video camera at the end, is inserted into a joint to evaluate and treat the condition.
The benefits of arthroscopy compared to the alternative, open shoulder surgery, are smaller incisions, minimal soft tissue trauma, less pain leading to faster recovery.
Multidirectional Shoulder Instability
Coming soon
Anterior Shoulder Instability
Coming soon
Posterior Shoulder Instability
Coming soon
Revision Repair with and Without Bone Loss
What is Triceps Repair?
Triceps repair is a surgical procedure that involves the repair of a ruptured (torn) triceps tendon. A tendon is a tough band of fibrous tissue which connects muscle to bone and works together with muscles in moving your arms, fingers, legs, and toes. The triceps tendons connect the triceps muscles to the shoulder blade and elbow in your arm. Rupture of the triceps tendon is a rare injury that occurs as a result of the detachment of the triceps tendon from the attached bone. These tendons can rupture with lifting heavy weights, during contact sports or after a fall on an outstretched arm.
Indications for Triceps Repair
Triceps repair is indicated for partial or complete rupture of the triceps tendons after trauma or injury. It is also indicated for repairing acute (injuries occurring within four weeks) or chronic (injuries occurring after four weeks) triceps tendon injuries. Distal triceps tendon rupture occurs due to the detachment of the triceps tendon connecting the triceps muscles to the elbow. These injuries require immediate medical attention and surgical repair to restore the activity of the triceps muscles.
Preparing for the Surgery
Your surgeon may order blood tests and other essential tests a few days before the surgery. Magnetic resonance imaging (MRI) may be suggested to examine parts of your arm, muscles and blood vessels. X-rays of your shoulder, elbow, and arms may be ordered. Your blood pressure, breathing rate, temperature, and heart rate will also be recorded. Your shoulder, arm, forearm, and elbow will be cleaned with soap and water and will be covered with sheets before the procedure.
Surgical Procedure
Medications through an intravenous line will be administered to help you relax. The procedure will be performed under general or regional anesthesia to keep you comfortable during the surgery.
- Your surgeon will make an incision behind the elbow and drill holes into the end of the ulna (bone in the forearm).
- The ends of the torn tendons will then be inserted through the holes and stitched. Your surgeon may also use screws and buttons to attach the tendon to the bone.
- For chronic tendon injuries, a tendon or a hard tissue from another part of the body may be used to lengthen the existing short tendon.
- After the tendon is attached to the bone, it is sutured and the incisions are closed with surgical tapes or bandages.
Post-operative Care
After the procedure, a cast or splint is placed on the elbow to prevent movement and protect the tendon while it heals. After 6 to 8 weeks of surgery, your physical therapist will teach you exercises to be performed at home for improving strength and range of motion in your arm. Contact your doctor if you have fever, swelling, redness, or drainage from the incision.
Risks and Complications
As with any surgical procedure, triceps repair involves certain potential risks and complications. They include:
- Bleeding and infection at the surgical site
- Damage to the other parts of the arm, such as muscles, bones, nerves or blood vessels
- Restricted movement of the arm
- Difficulty in resuming usual activities or sports
Multi-directional Instability(MDI)
Coming soon
Anterior Instability
Coming soon
Posterior Instability
Coming soon
Fresh Blood Imaging
Coming soon
Other Shoulder Condition Topics:
- Acromioclavicular (AC) Joint Osteoarthritis
- Baseball and Shoulder Injuries
- Rotator Cuff Pain
- Massive Retracted Rotator Cuff Tear
- Bicep Tendon Rupture
- Proximal Biceps Tendon Rupture
- Long Head Biceps Tendon Rupture
- Proximal Biceps Tendinitis
- Shoulder Pain
- Internal Impingement of the Shoulder
- Sternoclavicular Joint (SC joint)
- SLAP Tears
- Arthritis of the Shoulder
- Shoulder Labral Tear
- Shoulder Labral Tear with Instability
- Shoulder Dislocation
- Shoulder Trauma
- Subluxation
- Little League Shoulder
- Frozen Shoulder
- Clavicle Fracture
- Glenoid Fractures
- Proximal Humerus Fractures
- Shoulder Disorders
- Hill-Sachs Lesion
- Thrower’s Shoulder
- Overhead Athlete’s Shoulder
- Snapping Scapula
- Shoulder Instability
- Shoulder Impingement
- Rotator Cuff Tear
- Acromioclavicular Joint Injury
- Shoulder Fracture
- Scapula Injury
- Biceps Tunnel Disease
- AC Joint Injury
- Revision RC Repair
- Revision Repair








